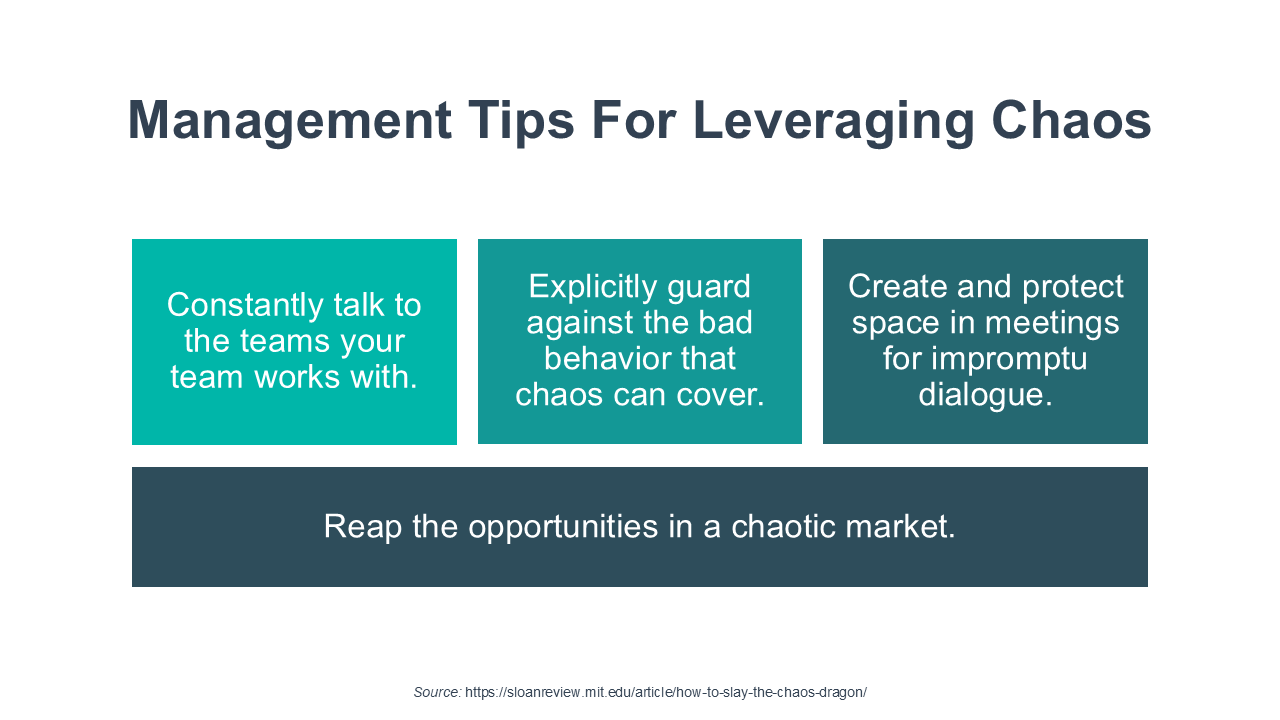
Chaos is here to stay, and executives need to adjust their leadership and management practices to adapt. That was the theme of a recent article—How To Slay The Chaos Dragon. And it makes me tired. The authors argue that chaos has become a permanent feature of modern organizations—driven by external volatility, shifting priorities, operational complexity, and constant market change.
Our recent coverage of new developments in the field illustrates the chaotic environment that executives need to lead through. Just in the past couple weeks, we’ve seen changes in rates (see CareSource Georgia Cuts Medicaid ABA Rates 20% and …
-
Management Newsletter Issue
|
Referral Development In The Age Of AI: The OPEN MINDS Management Newsletter, May 2026
-
Market Intel Report
|
Medicaid Foster Care Enrollment Updates, 2022-2024: An OPEN MINDS Market Intelligence Report
-
Innovative Program Profile
|
The PASSE Program By CareSource: An OPEN MINDS Program Profile
RFPs
- Missouri Seeks Transitional Living Program Services
- Missouri Seeks Health, Hunger & Hygiene Services
- Michigan’s Ottawa County Seeks Public Defender Services For Delinquency & Neglect/Abuse Cases
- California Seeks Electronic Medication Administration Record Software Subscription & Training Services
- New York Seeks SNUG Motivational Interviewing Services
- Texas Seeks Third-Party Medicaid Billing Services
- Kentucky Seeks Comprehensive Street Outreach Services
- Florida’s St. Johns County Seeks Medical Examiner Forensic Database Application Services
- Illinois’ Village Of Oak Park Seeks Workers Compensation Claims Administration Services
- Connecticut Seeks Limited Secure Services
Contract Awards
- North Carolina Awards Five Rural Organizations Orchestrating Transformation For Sustainability (NC ROOTS) Hubs Contracts
- Nevada Awards Medical Clinics For Telemedicine Kiosk Services Contract To OnMed, LLC
- Iowa Awards Trauma Informed Care Services Contract To Lutheran Services In Iowa
- Nevada Awards Virtual Early Childhood Family Engagement Program Services Contract To Waterford Institute
- Nevada Awards Multiple Coordination Only Dual Eligible Special Needs Plans (CO D-SNP) Program Services Contracts
Winning Proposals
- North Carolina Awards Five Rural Organizations Orchestrating Transformation For Sustainability (NC ROOTS) Hubs Contracts
- Hawaii Awards Community Care Services Program That Provides Behavioral Health Services To Medicaid Eligible Adults Who Have A Serious Mental Illness (SMI) Or Serious Persistent Mental Illness (SPMI) Contract To AlohaCare
- Nevada Awards Medical Clinics For Telemedicine Kiosk Services Contract To OnMed, LLC
- Federal Government Awards 988 Suicide & Crisis Lifeline Administrator Services Contract To Mental Health Association Of New York City, Inc.
- Colorado’s El Paso County Awards Domestic & Sexual Violence Services Contract To TESSA Of Colorado Springs
On-Demand Webinars & Executive Roundtables
- Breaking Down Silos: How One State Achieved 98% Faster Referral Response With Integrated Data & Coordination Tools
- Fortifying Your Strategic Vision With The Right Technological Infrastructure
- From Referral To Admission: How Automation Transforms Intake
- Federal Policy Meets Clinical Innovation: A Conversation With ASTP/ONC
- From Survival To Sustainability: Creating A Winning Strategy In An Unstable Market
Institute Presentations
- Preparing For Impact: Performance Management As A Financial Sustainability Tool
- Building Stability In Behavioral Health Through Care Delivery With RevDoc– Sponsored By RevDoc
- Reclaiming Time For Care: AI Documentation That Expands Capacity
- The Great Divide: Bridging The Gap Between Clinical & Financial Executives
- From Portals To Participation: Provider Insights On Digital Engagement, Adoption & Performance– Sponsored By Cantata Health Solutions
Market Intelligence Reports
- Medicaid Foster Care Enrollment Updates, 2022-2024: An OPEN MINDS Market Intelligence Report
- Medicaid Demonstration & Care Management Waivers: An OPEN MINDS Market Intelligence Report
- Trends In Affordable Care Act Health Insurance Marketplace Enrollment: An OPEN MINDS Market Intelligence Report
- Medicaid Home & Community-Based Services Waivers Covering The I/DD Population: An OPEN MINDS Market Intelligence Report
- Medicaid Care Coordination Initiatives—A State-By-State Guide: An OPEN MINDS Market Intelligence Report
Upcoming Executive Events
Upcoming Institutes
-
The 2026 OPEN MINDS Strategy & Innovation Institute
June 09 – June 11, 2026 – New Orleans, Louisiana
-
The 2026 OPEN MINDS Service Excellence Institute
August 11 – August 13, 2026 – San Francisco, California
-
The 2026 OPEN MINDS Executive Leadership Retreat
September 29 – October 01, 2026 – Gettysburg, Pennsylvania
-
The 2026 OPEN MINDS Technology & Analytics Institute
October 27 – October 29, 2026 – Philadelphia, Pennsylvania
-
The 2027 OPEN MINDS Performance Management Institute
February 16 – February 18, 2027 – Clearwater Beach, Florida
Upcoming Executive Summits
-
The 2026 OPEN MINDS Autism & I/DD Summit
June 10, 2026 – New Orleans, Louisiana -
The 2026 OPEN MINDS Government Health & Human Services Executive Summit
June 11, 2026 – New Orleans, Louisiana -
The 2026 OPEN MINDS Aging Services & Supports Summit
August 12, 2026 – San Francisco, California -
The 2026 OPEN MINDS Health & Human Services Workforce Best Practices Summit
September 30, 2026 – Gettysburg, Pennsylvania -
The 2026 OPEN MINDS CFO Summit
October 1, 2026 – Gettysburg, Pennsylvania -
The 2026 OPEN MINDS CEO Tech & AI Summit
October 28, 2026 – Philadelphia, Pennsylvania -
The 2026 OPEN MINDS Addiction & SUD Summit
October 29, 2026 – Philadelphia, Pennsylvania -
The 2027 OPEN MINDS Whole Person Care Summit
February 17, 2027 – Clearwater Beach, Florida -
The 2027 OPEN MINDS Workforce AI Summit
February 18, 2027 – Clearwater Beach, Florida
Upcoming Best Practice Seminars
-
MA&A Strategy For A Shifting Market: The 2026 OPEN MINDS Seminar On Planning & Succeeding in Increasing Scale
June 9, 2026 – Virtual Event -
Improving Consumer Experience: The 2026 OPEN MINDS Executive Seminar On Creating Better Engagement & Increasing Revenue
June 9, 2026 – New Orleans, Louisiana -
Optimizing Health Plan Contracting: The 2026 OPEN MINDS Executive Seminar On Building Referrals, Revenue & Margins
August 11, 2026 – San Francisco, California -
Portfolio Management To Optimize Organizational Performance: The 2026 OPEN MINDS Executive Seminar On How To Build A Service Line Portfolio For the Future
August 11, 2026 – San Francisco, California -
Strategic Planning For Times Of Uncertainty: The 2026 OPEN MINDS Seminar On Nimble Data-Driven Planning
September 29, 2026 – Gettysburg, Pennsylvania -
Finding An EHR For Your Future: The 2026 OPEN MINDS Best Practices Seminar On EHR Selection, Implementation & Optimization
October 27, 2026 – Philadelphia, Pennsylvania -
Creating A Winning Tech Strategy: The 2026 OPEN MINDS Seminar On Building A Digital Transformation Roadmap
October 27, 2026 – Philadelphia, Pennsylvania -
Building A Data-Driven Organization: The 2027 OPEN MINDS Seminar On Making Metrics-Based Management Work
February 16, 2027 – Clearwater Beach, Florida -
Measuring & Managing Financial Strength: The 2027 OPEN MINDS Seminar On A Framework For Improving Financial Resilience
February 16, 2027 – Clearwater Beach, Florida
Upcoming Webinars
-
Breaking Through Adoption Barriers In Evidence-Based SUD Treatment: How KCS Health Center Expanded From Basic Access To A Fully Integrated “SUD 2.0” Model
June 16, 2026 – Virtual Event -
Beyond Ambient: An AI Governance Framework For Behavioral Health Leaders
June 18, 2026 – Virtual Event
Upcoming Circle Elite Executive Roundtables
-
Transforming Adolescent Residential Services: The New Hope Case Study
June 1, 2026 – Virtual Event -
Designing A Measurable, Outcome-Driven Value-Based Care Model: The Community Health Network (MyCHN) Case Study
June 15, 2026 – Virtual Event -
Technology As Capacity & Quality Multiplier: The Monarch Case Study
June 22, 2026 – Virtual Event -
Correcting The Mistakes That Undermine Strategy Execution: The Adelphoi Case Study
June 29, 2026 – Virtual Event -
Turning AI Into Clinical Advantage: The Christian Children’s Home of Ohio Case Study
July 20, 2026 – Virtual Event -
Building A Crisis Response Ecosystem: The Connections Health Solutions Case Study
July 27, 2026 – Virtual Event -
Building A Culture Of Safety To Transform Care: The Traumatic Stress Institute & RWJBarnabas Health Case Study
August 3, 2026 – Virtual Event -
Building A Crisis Response Ecosystem: The Connections Health Solutions Case Study
August 17, 2026 – Virtual Event
Innovative Program Profiles
- Career Pathway Connections By Easterseals New Jersey: An OPEN MINDS Program Profile
- The PASSE Program By CareSource: An OPEN MINDS Program Profile
- Family Centered Treatment (FCT) By Pressley Ridge: An OPEN MINDS Program Profile
- Structured Psychotherapy for Adolescents Responding to Chronic Stress (SPARCS) By OMNI: An OPEN MINDS Program Profile
- The Seven Challenges Program By OMNI: An OPEN MINDS Program Profile
News Wire
- U.S. Begins Revoking Passports For Individuals Owing $100,000+ In Child Support Debt
- Health Care Chapter 11 Bankruptcies Increased 33% In First Quarter 2026
- Individuals With ADHD & SUD Nearly Twice As Likely To Stop ADHD Medication Within One Year
- Children With Chronic Health Conditions & Social Needs Had More Than Five Times The Rate Of Elevated School Absenteeism
- Payments For At Least 16% Of Medicare Virtual Check-Ins Potentially Improper; E-Visit Error Rate Was At Least 2.6%
- One-Third Of Adolescents With Autism Meet One Or More Criteria For Profound Autism
- Commercially Insured Individuals Wait An Average Of 50 Days For First Neurologist Appointment
Market Updates
- BranchLab Raises $26 Million In Series A Financing For Its AI Platform To Commercialize Pharmaceuticals
- Cantex & Headlamp Health Partner On AI For Precision Neuropsychiatry To Support Clinical Drug Development
- Easterseals Florida Launches Mental Health Clinic In Sorrento
- Providence Health Plan In The Pacific Northwest To Wind Down Insurance Business
- St. Christopher’s Hospital For Children In North Philadelphia Announces Layoffs Ahead Of Kidney Transplant Program Closure
Management Newsletter
Industry Resources
- Provisional Drug Overdose Death Counts
- Dear Colleague Letter
- ARHOME Section 1115 Demonstration Project Application
- CMS Could Strengthen Medicare Program Safeguards To Prevent & Detect Potentially Improper Payments For Virtual Check-In & E-Visit Services
- Maryland Senate Bill 323 Juvenile Court – Jurisdiction, Detention & Confinement (Youth Charging Reform Act)
- Contract Year 2027 Medicare Advantage & Part D Final Rule
- Bessey v. Nebraska